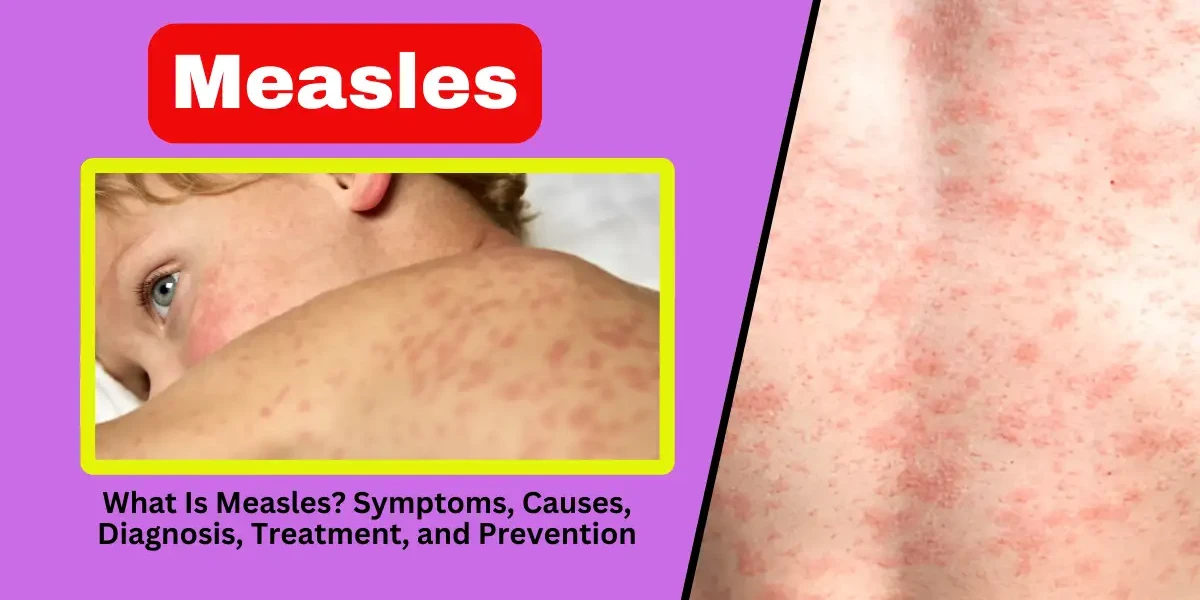
Measles, also known as rubeola, is one of the most contagious viral infections known to humankind. Before the introduction of the measles vaccine in 1963, the disease caused millions of deaths annually, particularly among young children. Despite being vaccine-preventable, measles remains a significant global health threat, especially in regions with low immunization rates. The World Health Organization (WHO) estimates that measles caused over 128,000 deaths worldwide in 2021, mostly in unvaccinated or under-vaccinated populations.
Measles is an acute viral infection caused by the measles virus (MeV), a single-stranded RNA virus belonging to the Morbillivirus genus in the Paramyxoviridae family. It is exclusively a human disease, meaning it does not infect animals, and humans are the only natural hosts. The virus spreads through respiratory droplets when an infected person coughs or sneezes, and it can remain infectious in the air or on surfaces for up to two hours.
The measles virus primarily targets the respiratory system before spreading to other organs, including the skin, eyes, and lymphatic system. It suppresses the immune system, making infected individuals more susceptible to secondary bacterial infections such as pneumonia and otitis media (ear infections). Before vaccination became widespread, nearly every child contracted measles by age 15. Today, outbreaks still occur in unvaccinated communities, often leading to severe complications, especially in malnourished children, pregnant women, and immunocompromised individuals.
One of the most concerning aspects of measles is its high contagion rate. An infected person can spread the virus to 12–18 other people in a susceptible population, making it far more infectious than COVID-19 or influenza. This is why herd immunity (vaccination rates of at least 95%) is crucial to preventing outbreaks.
There are two main types of measles:
Rubeola (Standard Measles) – The most common form, characterized by a distinctive rash, high fever, and respiratory symptoms.
Rubella (German Measles) – A milder viral infection caused by a different virus. Though sometimes confused with rubeola, rubella is less severe but dangerous for pregnant women due to the risk of congenital rubella syndrome.
This article focuses on rubeola, the classic form of measles.
Measles, also known as rubeola, is a highly contagious viral infection that primarily affects the respiratory system and then spreads throughout the body. The disease progresses through distinct stages, each with its own set of symptoms. Understanding these signs is crucial for early diagnosis, treatment, and prevention of complications. Below, I will explain the symptoms and signs of measles in detail, covering the progression from early infection to recovery or potential complications.
After being exposed to the measles virus, there is an incubation period of about 10 to 14 days before symptoms appear. During this time, the virus multiplies in the respiratory tract and begins spreading to the lymph nodes. The patient does not exhibit any symptoms yet but is already contagious.
The first signs of measles resemble those of a severe cold or flu. These early symptoms include:
High Fever (Often Spiking Up to 104°F or 40°C): The fever is one of the first and most prominent symptoms, usually lasting several days.
Cough (Dry, Persistent): A hacking cough develops due to inflammation in the respiratory tract.
Runny Nose (Coryza): Nasal congestion and clear discharge are common, similar to a cold.
Red, Watery Eyes (Conjunctivitis): The eyes become inflamed, sensitive to light (photophobia), and may produce a thick discharge.
Koplik’s Spots (Pathognomonic Sign): These are small, white, bluish-gray spots with a red base that appear on the inner cheeks (buccal mucosa) near the molars. They usually appear 1-2 days before the rash and are a definitive sign of measles.
The characteristic measles rash is a maculopapular eruption (flat red spots with small bumps) that begins on the face and behind the ears before spreading downward to the neck, chest, arms, legs, and feet. Key features of the rash include:
Starts at the Hairline and Face: The rash first appears as faint pink spots that gradually darken and merge into larger blotches.
Spreads Centrifugally (Head to Toe): Over 2-3 days, it covers most of the body, including the palms and soles.
Fever Persists or Spikes Higher: The fever often peaks when the rash is at its worst.
Rash Lasts 5-7 Days: After reaching full coverage, the rash begins to fade in the same order it appeared (face first, then extremities), sometimes leaving a brownish discoloration or fine peeling of the skin.
Most patients begin to recover once the rash fades. The fever subsides, and energy levels gradually return to normal. However, the cough and fatigue may linger for a week or more. The immune system remains weakened for several weeks, increasing susceptibility to secondary infections like pneumonia or ear infections.
While most healthy individuals recover fully, measles can lead to severe complications, especially in:
Infants and young children
Malnourished individuals
Pregnant women
Immunocompromised patients (e.g., those with HIV or leukemia)
Measles can escalate rapidly, so prompt medical evaluation is necessary if:
The fever exceeds 104°F (40°C) or persists beyond the rash phase.
Difficulty breathing or chest pain develops (signs of pneumonia).
Severe headache, confusion, or seizures occur (possible encephalitis).
Dehydration (reduced urination, dry mouth, lethargy) is observed.
Measles, also known as rubeola, is a highly contagious viral infection that primarily affects the respiratory system before spreading throughout the body. It is caused by the measles virus, a member of the Morbillivirus genus in the Paramyxoviridae family. This virus is exceptionally efficient at spreading from person to person, making it one of the most infectious diseases known. To fully understand how measles develops and who is most vulnerable, we must examine its causes and risk factors in depth.
The measles virus (MeV) is the sole cause of measles, meaning no other pathogen can produce this specific illness. This virus is an RNA virus, which means its genetic material is composed of ribonucleic acid, allowing it to mutate slightly over time, though not as rapidly as influenza or SARS-CoV-2. The measles virus primarily targets the immune system, specifically dendritic cells, macrophages, and lymphocytes, which are crucial for defending the body against infections.
How the Measles Virus Spreads
The virus is transmitted through respiratory droplets when an infected person coughs, sneezes, or even talks. These droplets can remain suspended in the air for up to two hours, making measles one of the most contagious diseases—far more so than influenza or the common cold. Additionally, the virus can survive on contaminated surfaces, allowing indirect transmission if a person touches an infected surface and then their mouth, nose, or eyes.
Once inside the body, the virus replicates in the respiratory tract before entering the bloodstream (viremia), spreading to lymph nodes, the spleen, and other organs. The incubation period—the time between exposure and symptom onset—is typically 10 to 14 days, during which an infected person may unknowingly spread the virus to others.
While anyone exposed to the measles virus can contract the disease, certain factors significantly increase the likelihood of infection and severe complications. These include:
1. Lack of Vaccination (Most Significant Risk Factor)
The measles-mumps-rubella (MMR) vaccine is highly effective (about 97% protection after two doses) in preventing measles. However, individuals who are unvaccinated or undervaccinated (missing one or both doses) are at the highest risk. Vaccine hesitancy, misinformation, and lack of access to immunization programs contribute to outbreaks.
Infants too young for vaccination (under 12 months) rely on herd immunity for protection.
People with compromised immune systems (e.g., leukemia, HIV, or chemotherapy patients) may not respond well to the vaccine.
2. Travel to or Residence in Areas with Measles Outbreaks: Measles remains endemic in many parts of the world, particularly in regions with low vaccination rates, such as parts of Africa, Asia, and Eastern Europe. Travelers to these areas, including tourists and healthcare workers, are at increased risk of exposure.
3. Crowded or Close-Contact Environments: The virus spreads rapidly in settings where people are in close quarters, such as:
Schools and daycare centers (especially among unvaccinated children)
Refugee camps and homeless shelters (due to poor sanitation and overcrowding)
Hospitals and clinics (healthcare workers may encounter infected patients)
4. Weakened Immune System (Immunocompromised Individuals): People with HIV/AIDS, cancer patients undergoing chemotherapy, or those on immunosuppressive drugs (e.g., for autoimmune diseases) are at higher risk for severe measles complications, such as pneumonia or encephalitis.
5. Pregnancy-Related Risks: Pregnant women who contract measles face higher risks of premature birth, low birth weight, or even maternal death. Additionally, they cannot receive the live MMR vaccine during pregnancy due to potential risks to the fetus.
6. Vitamin A Deficiency: Studies show that vitamin A deficiency is linked to more severe measles cases, including a higher risk of blindness and death. Vitamin A plays a crucial role in immune function and epithelial tissue integrity, which the measles virus damages.
7. Age-Related Susceptibility
Infants (under 5 years old) have immature immune systems, making them prone to severe complications like pneumonia or encephalitis.
Adults (over 20 years old) who contract measles may experience more severe symptoms than children, possibly due to a stronger immune response leading to higher fever and inflammation.
8. Previous Measles Infection Does Not Guarantee Lifelong Immunity
While most people develop lifelong immunity after recovering from measles, rare cases of reinfection have been reported, particularly in individuals with weakened immune systems.
Measles, also known as rubeola, is a highly contagious viral infection caused by the measles virus. The disease progresses through several distinct stages, each with its own set of symptoms and characteristics. Understanding these stages helps in early diagnosis and proper management of the illness.
1. Incubation Period (7–14 Days After Exposure)
The incubation period is the time between exposure to the virus and the appearance of the first symptoms. During this stage, the virus multiplies in the respiratory tract and spreads to the lymph nodes. Infected individuals do not show any symptoms yet but can still transmit the virus to others. This stage typically lasts between 7 to 14 days, with an average of 10–12 days before symptoms become noticeable.
2. Prodromal Stage (Initial Symptoms: 2–4 Days Before Rash Appears)
The prodromal stage marks the beginning of noticeable symptoms. Common early signs include high fever (often exceeding 104°F or 40°C), cough, runny nose (coryza), red and watery eyes (conjunctivitis), and small white spots inside the mouth called Koplik’s spots (pathognomonic for measles). Fatigue, loss of appetite, and general malaise are also common. This stage is highly contagious, and the virus spreads through respiratory droplets when an infected person coughs or sneezes.
3. Acute (Rash) Stage (Lasts About 5–7 Days)
The characteristic measles rash typically appears 3–5 days after the initial symptoms. It begins as flat red spots on the face (especially behind the ears and along the hairline) and gradually spreads downward to the neck, torso, arms, legs, and feet. The rash may merge into larger blotchy patches and is often accompanied by a persistent high fever. The rash usually lasts for about 5–7 days before fading in the same order it appeared (from head to feet). During this phase, the patient remains highly contagious.
4. Recovery Stage (1–2 Weeks After Rash Appears)
As the immune system fights off the virus, the fever subsides, and the rash begins to fade, turning brownish and eventually peeling off in some cases. Cough and fatigue may persist for several days to weeks. The patient’s contagiousness decreases significantly after the rash has been present for at least four days. However, the immune system may remain weakened for weeks, increasing susceptibility to secondary infections like pneumonia or ear infections.
5. Possible Complications (Can Occur in High-Risk Groups)
While most people recover fully, measles can lead to severe complications, especially in young children, malnourished individuals, and those with weakened immune systems. Common complications include pneumonia, encephalitis (brain inflammation), severe diarrhea leading to dehydration, and in rare cases, subacute sclerosing panencephalitis (SSPE), a fatal neurological disorder that develops years after infection. Vaccination is the most effective way to prevent measles and its complications.
Diagnosing measles involves a combination of clinical evaluation, patient history, and laboratory testing. Since measles symptoms can resemble other viral infections, accurate diagnosis is essential for proper treatment and public health measures.
Measles typically begins with high fever, cough, runny nose, and red, watery eyes (conjunctivitis). After a few days, small white spots called Koplik spots may appear inside the mouth, which are a key early sign. A red, blotchy rash then develops, starting on the face and spreading downward to the rest of the body. The rash usually lasts about a week. Doctors assess these symptoms alongside exposure history, such as contact with infected individuals or travel to areas with measles outbreaks.
To confirm a measles diagnosis, laboratory tests are often necessary. These include:
RT-PCR (Reverse Transcription Polymerase Chain Reaction): Detects measles virus RNA in throat or nasal swabs, urine, or blood samples. This is the most reliable method, especially in the early stages.
Serology (IgM Antibody Test): Checks for measles-specific IgM antibodies in the blood, which appear shortly after infection. This test is most effective 3–4 days after the rash appears.
Viral Culture: Rarely used due to its slow turnaround time, but it can isolate the live virus from patient samples.
Since measles symptoms overlap with other illnesses, doctors must rule out conditions like rubella, scarlet fever, dengue, roseola, or allergic reactions. The presence of Koplik spots, the progression of the rash, and lab testing help distinguish measles from similar diseases.
Measles is a notifiable disease, meaning confirmed or suspected cases must be reported to health authorities. This helps track outbreaks, implement quarantine measures, and initiate vaccination campaigns to prevent further spread.
Early diagnosis is crucial to managing complications (like pneumonia or encephalitis) and preventing transmission, especially in unvaccinated populations. Immunization continues to be the strongest safeguard against measles.
Measles, also known as rubeola, is a highly contagious viral infection caused by the measles virus. While there is no specific antiviral treatment for measles, management focuses on supportive care, prevention of complications, and, in some cases, the use of medications to alleviate symptoms. The cornerstone of treatment includes ensuring proper hydration, rest, and fever control. Since measles weakens the immune system, secondary bacterial infections such as pneumonia or ear infections may occur, requiring antibiotics. Vitamin A supplementation is strongly recommended, particularly in children, as it has been shown to reduce the severity of the disease and decrease mortality rates. In severe cases, especially among immunocompromised individuals, ribavirin (an antiviral) or intravenous immunoglobulins (IVIG) may be considered, though evidence supporting their efficacy remains limited. The best strategy against measles is prevention through vaccination with the measles-mumps-rubella (MMR) vaccine, which provides lifelong immunity in most cases. Below, we will explore in detail the treatment and medication options for measles, including supportive measures, pharmacological interventions, and preventive strategies.
Since measles is a viral infection, antibiotics are ineffective against the virus itself. Treatment mainly revolves around relieving symptoms and preventing complications. Patients should be isolated to prevent the spread of the disease, as measles is transmitted through respiratory droplets and can remain infectious in the air for up to two hours.
1. Hydration and Nutrition
Dehydration is a common concern, especially in children, due to fever and reduced fluid intake. Oral rehydration solutions (ORS) or increased water intake are essential. If a patient is unable to drink adequately, intravenous (IV) fluids may be necessary. Proper nutrition is also crucial, as malnutrition can worsen measles outcomes.
2. Fever and Pain Management
High fever is a hallmark of measles and can be managed with antipyretics such as:
Acetaminophen (Paracetamol): The preferred choice for reducing fever and relieving pain, especially in children.
Ibuprofen: An alternative for older children and adults, though it should be used cautiously in those with stomach ulcers or kidney issues.
Avoid aspirin in children and teenagers due to the risk of Reye’s syndrome, a rare but serious condition that causes liver and brain damage.
3. Vitamin A Supplementation
Vitamin A deficiency is linked to more severe measles cases and higher mortality. The World Health Organization (WHO) recommends the following doses for children with measles:
50,000 IU for infants < 6 months
100,000 IU for infants 6–11 months
200,000 IU for children ≥ 12 months
A second dose should be given 24 hours later, and a third dose after 4 weeks for children with clinical signs of vitamin A deficiency.
While measles itself does not have a direct antiviral treatment, secondary bacterial infections are common and require antibiotics.
1. Antibiotics for Bacterial Superinfections
Pneumonia: A frequent complication, often requiring antibiotics like amoxicillin or, in severe cases, intravenous ceftriaxone.
Otitis media (ear infection): Treated with amoxicillin-clavulanate or azithromycin if penicillin-allergic.
Conjunctivitis: If bacterial, topical or oral antibiotics may be prescribed.
2. Antiviral and Immunomodulatory Therapies (Rare Cases)
Ribavirin: An antiviral that has been used experimentally in severe measles cases, particularly in immunocompromised patients, though data is limited.
Intravenous Immunoglobulins (IVIG): May be given to exposed high-risk individuals (e.g., unvaccinated pregnant women, immunocompromised patients) within six days of exposure to prevent or lessen infection.
Most healthy individuals recover fully within 2–3 weeks.
Complications occur in 30% of cases, more frequently in:
Children under 5
Adults over 20
Malnourished or immunocompromised patients
Mortality rate:
0.1–0.2% in developed countries with good healthcare.
Up to 10% in malnourished populations.
The cornerstone of measles prevention is the measles-mumps-rubella (MMR) vaccine, which is highly effective (about 97% protection after two doses). The vaccine contains live attenuated (weakened) measles virus, which stimulates the immune system to produce antibodies without causing the disease.
Vaccination Schedule:
First dose: Given at 12-15 months of age.
Second dose: Administered at 4-6 years (or at least 28 days after the first dose).
Catch-up vaccination: Unvaccinated older children and adults should receive two doses at least 28 days apart.
Herd Immunity: When a high percentage of the population (about 95% or more) is vaccinated, community transmission is significantly reduced, protecting those who cannot be vaccinated (e.g., infants under 12 months, pregnant women, or immunocompromised individuals).
If an unvaccinated person is exposed to measles, certain interventions can reduce the risk of infection or severity:
MMR Vaccine (Within 72 Hours of Exposure): If given promptly, the vaccine may prevent or modify the disease course.
Immune Globulin (Within 6 Days of Exposure): Recommended for high-risk individuals (infants <12 months, pregnant women, immunocompromised patients) who cannot receive the live vaccine.
Since measles spreads via respiratory droplets (coughing, sneezing) and can remain infectious in the air for up to two hours, infection control is critical:
Isolation of infected individuals (for at least 4 days after rash onset).
Use of masks and proper hand hygiene to reduce transmission.
Quarantine for exposed, unvaccinated individuals for up to 21 days (the incubation period of measles).
Public health authorities monitor measles cases to prevent outbreaks through:
Contact tracing to identify and vaccinate exposed individuals.
Public awareness campaigns to promote vaccination.
Travel-related precautions, as measles is still endemic in many countries.
While most people recover from measles without major issues, about 30% of cases develop complications, which can be severe or even fatal. Complications are more common in:
Children under 5 years old
Adults over 20 years old
Pregnant women (risk of preterm birth or low birth weight)
Malnourished or vitamin A-deficient individuals
Immunocompromised patients (e.g., HIV/AIDS, leukemia, chemotherapy recipients)
Pneumonia (Most Common Cause of Measles-Related Deaths):
Can be viral (direct measles infection of lungs) or bacterial (secondary infection by Streptococcus pneumoniae or Staphylococcus aureus).
Symptoms: High fever, difficulty breathing, chest pain.
Treatment: Antibiotics for bacterial pneumonia, supportive care (oxygen, fluids).
Laryngotracheobronchitis (Croup):
Inflammation of the upper airways leading to a barking cough and stridor.
May require steroids or hospitalization in severe cases.
Acute Encephalitis (1 in 1,000 Cases):
Inflammation of the brain, occurring 1-2 weeks after rash onset.
Symptoms: High fever, seizures, confusion, coma.
Mortality: 10-15%, with 25% of survivors having permanent brain damage (e.g., epilepsy, intellectual disability).
Subacute Sclerosing Panencephalitis (SSPE) (Rare but Fatal):
A delayed complication occurring 7-10 years after measles infection.
Caused by persistent measles virus in the brain.
Symptoms: Behavioral changes, cognitive decline, seizures, muscle spasms, coma.
No cure; fatal within 1-3 years of symptom onset.
Diarrhea and Dehydration:
Common in young children, leading to severe fluid loss.
May require oral rehydration therapy (ORT) or IV fluids.
Stomatitis (Mouth Ulcers):
Painful sores making eating/drinking difficult.
Keratitis (Corneal Inflammation):
Can lead to corneal scarring and blindness, especially in vitamin A-deficient individuals.
Treatment: High-dose vitamin A supplementation reduces severity.
Increases risk of:
Miscarriage
Preterm birth
Low birth weight
No evidence of congenital measles syndrome (unlike rubella).
Measles weakens the immune system for months to years, increasing susceptibility to other infections (e.g., tuberculosis, bacterial pneumonia).
Studies show 11-73% of immune memory cells are erased, requiring revaccination for some diseases.
Globally, ~140,000 deaths annually (mostly unvaccinated children in developing countries).
Case fatality rate:
0.1-0.2% in healthy, well-nourished populations.
Up to 10% in malnourished or immunocompromised groups.
Measles is a preventable yet dangerous disease. Thanks to vaccines, cases have plummeted, but outbreaks still happen where vaccination rates drop. Recognizing measles symptoms early, ensuring vaccination, and understanding treatment and prevention can save lives.
If you suspect measles, seek medical attention immediately—especially if you or your child are unvaccinated. Stay informed, stay protected, and help keep this ancient scourge at bay.
High fever (often over 104°F or 40°C)
Dry cough and runny nose
Red, watery eyes (conjunctivitis)
Koplik’s spots (tiny white spots inside the mouth)
A red, blotchy rash that starts on the face and spreads downward
Get the MMR (measles, mumps, rubella) vaccine (two doses are 97% effective).
Avoid close contact with infected individuals.
Practice good hygiene (washing hands frequently).
Isolate infected individuals to prevent spread.
Apply calamine lotion or oatmeal baths to soothe the skin.
Take antihistamines (like Benadryl) if approved by a doctor.
Keep the skin moisturized with fragrance-free lotion.
Avoid scratching to prevent infection.
Rest and stay hydrated.
Take acetaminophen (Tylenol) or ibuprofen for fever and pain.
Use a humidifier to ease cough and sore throat.
Get plenty of vitamin A (may help reduce complications).
Seek medical care if severe symptoms develop (e.g., difficulty breathing).
There is no cure for measles, but supportive care helps recovery:
Vitamin A supplements (recommended by WHO for faster recovery).
Fever reducers and hydration.
Rest in a dimly lit room (light sensitivity is common).
Symptoms appear 7–14 days after exposure.
Fever and rash typically last 5–7 days.
Full recovery may take 2–3 weeks.
Yes, but use lukewarm water (hot water can worsen itching).
Avoid harsh soaps; use mild cleansers.
Pat skin dry gently to avoid irritation.
Blood test (checks for measles antibodies).
Throat or nasal swab (PCR test for the virus).
Urine test (sometimes used to detect the virus).
"3-day measles" usually refers to rubella (German measles), not classic measles.
Symptoms include:
Mild pink rash (lighter than measles rash).
Low-grade fever.
Swollen lymph nodes.
Yes, the rash can be itchy, but not as severely as chickenpox.
Seek medical help if the child has:
High fever (over 103°F or 39.4°C).
Difficulty breathing or persistent cough.
Rash with purple spots (could indicate bleeding).
Signs of dehydration (no tears, dry mouth, no urination).
Vaccinate (first MMR dose at 12–15 months, second at 4–6 years).
Avoid exposure to infected people.
Breastfeed (provides some immunity if the mother is vaccinated).
Keep unvaccinated babies away from outbreaks.